Compare drug prices at GoodRx.ca
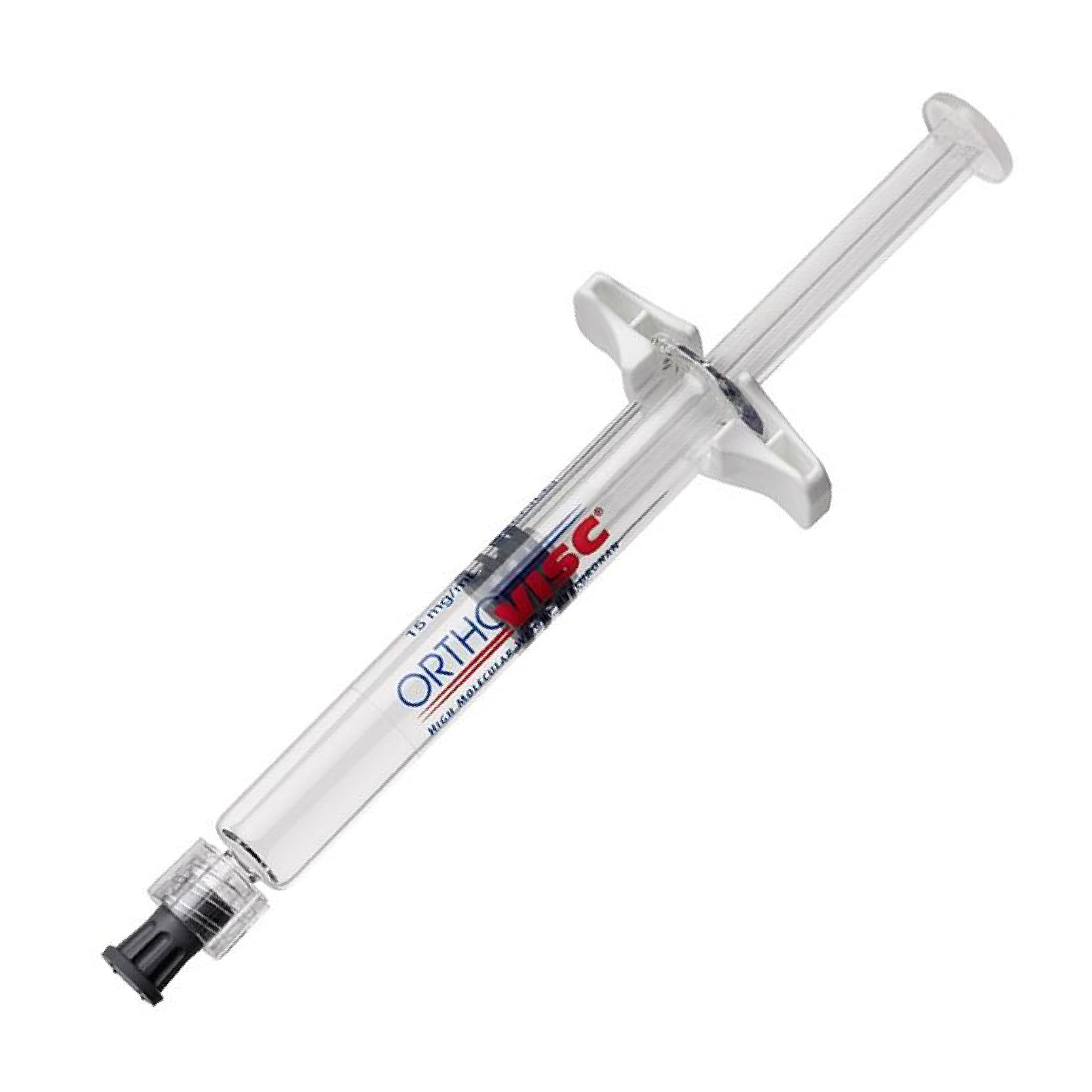
Orthovisc (Hyaluronic Acid) Syringe Injection – 3x2ml
US727.00
3x2ml
Brand Manufacturer: ANIKA THERAPEUTICS INC
Please click the currency converter flag in the top corner of the screen for the exchange rate from USD-CAD.
Compare CAD-USA drug prices at GoodRx.com
This order requires you to submit a prescription. Upload here. *Prescriptions on this website are fulfilled and from Canada and depending on the medication may originate from Australia, New Zealand United Kingdom, Canada or the United States. | Fulfillment policy See More.Description Of Product
Hyaluronate Derivatives, Amvisc/Durolane/Euflexxa/Gel-One/Healon/OrthoVisc/Provisc/Synvisc
Description: Antirheumatic, Orthopedics, Miscellaneous
How Does It Work
OrthoVisc/Provisc/Synvisc Work
Hyaluronic acid is a naturally occurring glycosaminoglycan polysaccharide and is the chief component of the extracellular matrix. Hyaluronic acid and its derivatives are highly anionic and attract water which results in volume expansion and structural support of soft tissues essentially functioning as tissue and joint lubricant improving the modulating interaction between adjacent tissues. When hyaluronic acid is used as an intra-articular injection increases the relative viscosity of the synovial fluid in cartilage. When administered as an intra-articular injection, the hyaluronic acid is cleared within several hours with half-lives ranging from 17 hours to 1.5 days. The half-life is longer for purified and synthesized hyaluronic acid preparations with a larger molecular weight. Despite such as short half-life, the clinical benefit of hyaluronic acid in providing significant symptomatic pain can be long-lasting following an intra-articular hyaluronic acid injection. More recently, studies have shown promising results in the treatment of tendinopathies which have been attributed to their anti-inflammatory activity, enhanced cell proliferation, collagen deposition besides the lubricating action on the sliding surface of the tendon.
Indications For Use
Intra-articular use if officially indicated for the treatment of pain in osteoarthritis. Various other indications for other formulations.
Precautions
Do not use in patients with a known hypersensitivity to hyaluronic acid or any components of its formulation
Do not use in a pre-existing infection of the skin region of the intended injection site
Do not use in patients with a systemic bleeding disorder
Should only be administered by a medical professional trained in accepted injection techniques
Usual Dosing
When administering by intra-articular injection, always refer to the manufacturer’s labelling for additional instructions on injection technique.
Injectable: According to the prescribed directions of a licensed medical doctor.
The following dosing recommendations are according to knee osteoarthritis:
Durolane: Inject 60 mg (3 mL) once.
Euflexxa: Inject 20 mg (2 mL) once weekly for 3 weeks (total of 3 injections).
Gel-One: Inject 30 mg (3 mL) once.
Gelson-3: Inject 16.8 mg (2 mL) once weekly for 3 weeks (total of 3 injections).
GenVisc 805, Supartz, Supartz FX: Inject 25 mg (2.5 mL) once weekly for 5 weeks (total of 5 injections); some patients may benefit from a total of 3 injections.
Hyalgan: Inject 20 mg (2 mL) once weekly for 5 weeks (total of 5 injections); some patients may benefit with a total of 3 injections.
Hymovis: Inject 24 mg (3 mL) once weekly for 2 weeks (total of 2 injections).
Monovisc: Inject 88 mg (4 mL) once.
Orthovisc: Inject 30 mg (2 mL) once weekly for 3 to 4 weeks (total of 3 to 4 injections).
Synvisc: Inject 16 mg (2 mL) once weekly for 3 weeks (total of 3 injections).
Synvisc-One: Inject 48 mg (6 mL) once.
Triluron: Inject 20 mg (2 mL) once weekly for 3 weeks (total of 3 injections).
Travis: Inject 25 mg (2.5 mL) once weekly for 3 weeks (total of 3 injections).
Visco-3: Inject 25 mg (2.5 mL) once weekly for 3 weeks (total of 3 injections).
Pharmacist Tips On Using
Hyaluronate Derivative Injection: Should be injected only into a joint and never extra-articular or into the synovial capsule or tissues. Do not use disinfectants containing ammonium salts for cleaning the injection site prior to administration. Should only be administered by a trained medical doctor.
Hyaluronate Derivative Should be Stored: Store this medication at 36°F to 77°F (2°C to 25°C) and away from heat, moisture, and light. Keep all medicine out of the reach of children. Throw away any unused medicine after the beyond-use date. Do not flush unused medications or pour down a sink or drain.
Side Effects
The type of local reaction may vary from product to product and site to site:
>10%:
Central Nervous System: Headache (≤18%)
Dermatologic: Skin discolouration at the injection site (4% to 78%), ecchymoses (≤14%), skin rash (≤14%)
Hematologic and Oncologic: Bruise (≤28%; more common in older patients)
Local: Swelling at the injection site (3% to 98%), tenderness at the injection site (17% to 95%), bruising at the injection site (3% to 93%), erythema at the injection site (≤93%), induration at the injection site (6% to 92%), pain at the injection site (≤92%), residual mass at the injection site (3% to 90%), itching at the injection site (7% to 47%), muscle rigidity at the injection site (25%), hematoma at the injection site (8% to 18%)
Neuromuscular and Skeletal: Arthralgia (1% to 25%), joint swelling (knee; ≤14%), joint effusion (≤11%)
Miscellaneous: Swelling (18% to 28%)
Special note for customers.
*All orders are limited to a 90 day supply. *Prescriptions on this website are fulfilled and from Canada and depending on the medication may originate from Australia, New Zealand United Kingdom, Canada or the United States.Disclaimer
All information contained in and provided by ZIPRx.ca is provided for educational purposes only. This information should not be used for the diagnosis or treatment of any health problem or disease. This information is not intended to replace clinical judgement or guide individual patient care in any manner. The User is hereby notified that the information contained herein may not meet the user’s needs. The User is advised that, although the information is derived from medical research and literature, we cannot guarantee either its correctness, comprehensiveness or currency. ZIPRx nor any of its affiliated parties shall be liable for any damage resulting in whole or part from any User’s use of or reliance upon the information contained within.Shipping Details
All orders received prior to 3:00 pm PST on business days will ship the following day; peak season and holiday shipping days may require an additional 24 hours. Our Pharmacy will make every effort to ship each order as quickly as possible. Orders received over the weekend will ship the following Monday as our shipping department is closed Saturday and Sunday. We offer shipping via Canada Post within Canada. We offer shipping via USPS and UPS within the continental United States and worldwide. Expedited shipping options are available at checkout if you want to receive your order sooner.Related products
Brand Name
Brand Name